Table of Contents
Understanding Insurance Coverage for ABA Therapy in Utah
Does insurance cover ABA therapy in Utah? Many families ask this vital question when seeking support for children with autism. Applied Behavior Analysis (ABA) therapy uses evidence-based techniques to enhance communication, social skills, and independence, making it essential for autism spectrum disorder management.
Since 2016, Utah’s law (SB 57, updated by SB 95 in 2019) mandates coverage for ABA under state-regulated plans like individual and fully insured large group policies, with no age or dollar caps. This includes options such as Utah Medicaid ABA therapy coverage and Tricare ABA therapy in Utah, often requiring medical necessity documentation and BCBA supervision. Private insurers, including ABA Therapy Cigna Utah, typically follow suit for eligible families.
At Golden Touch ABA Therapy, we guide you through insurance eligibility for autism behavioral therapy in Utah, verifying benefits and delivering personalized in-home sessions across counties. Like the Smith family in Salt Lake, who accessed ABA treatment funding through health plans in the state, we prioritize family-centered care with flexible scheduling to fit your life.
ABA Therapy Coverage Landscape in Utah
Navigating insurance for ABA therapy can feel overwhelming, but we’re here to guide families through the process with clear, supportive information. In Utah, state laws ensure strong support for children with autism, making essential treatments more accessible. This landscape includes private insurers, Medicaid, and Tricare, each offering pathways to in-home ABA therapy that focuses on family-centered care and measurable outcomes.
A common question is, does insurance cover ABA therapy in Utah? Yes, thanks to key legislation like SB 57, enacted in 2014 and effective from January 1, 2016, which mandates coverage for diagnosis and treatments including applied behavior analysis for individuals up to age 21 under individual and fully insured large group plans. The 2019 SB 95 further strengthened this by removing age and dollar caps, aligning with federal mental health parity laws. According to Autism Speaks, this has expanded access, with most private health plans now including ABA services alongside speech, occupational, and physical therapies, though small group plans may have exclusions based on employer specifics.
Private plans typically cover ABA based on medical necessity, but we recommend verifying benefits early to understand copays or prior authorizations. For families relying on public options, Utah Medicaid ABA therapy coverage plays a vital role through the Children’s Health Evaluation and Treatment (CHEC) program, which provides up to 40 hours weekly for eligible children under 21 with an autism diagnosis and income-based criteria, as outlined in state Medicaid guidelines. Military families can access Tricare ABA therapy in Utah via the Autism Care Demonstration, offering similar hour limits with age restrictions under 21 and required prior approvals.
Regional differences in Utah significantly impact access to autism behavioral intervention funding in Utah, especially for in-home services. Urban areas often have denser provider networks, while rural spots may require more coordination. Understanding these variations helps families choose the right support tailored to their location and needs, ensuring consistent therapy without unnecessary travel.
The following table compares insurance coverage aspects for ABA therapy in key Utah regions, highlighting eligibility, hour caps, and provider availability.
| Area/County | Primary Insurers Covering ABA | Typical Annual Hour Limits | Key Requirements | Provider Network Strength |
|---|---|---|---|---|
| Urban hub with broad access | High coverage under state mandate | Based on medical necessity | Standard documentation | Including Golden Touch ABA |
| Growing suburban area | Strong Medicaid integration | With progress monitoring | Income and diagnosis based | Dedicated local RBT teams |
| Northern rural access | Military family focus | Under Autism Care Demo | Prior authorization needed | Regional coverage available |
Data sourced from state Medicaid guidelines and Tricare policies for 2024. Hour limits vary by individual assessment; consult providers for specifics.
This comparison shows how health plan support for ABA services statewide can differ, with Salt Lake County offering the broadest options for a family navigating Medicaid approvals. In Utah County, for instance, aba therapy utah county benefits from growing suburban resources, easing scheduling for busy households. We at Golden Touch ABA bridge these gaps by assisting with benefits verification and creating personalized plans that maximize coverage, so every child receives evidence-based in-home ABA therapy without financial barriers holding them back.
For example, a Salt Lake family we supported recently used their private plan to secure 30 hours weekly, focusing on communication skills in a warm and welcoming environment. These tailored approaches highlight the power of small steps toward independence. As coverage evolves, staying informed empowers your journey.
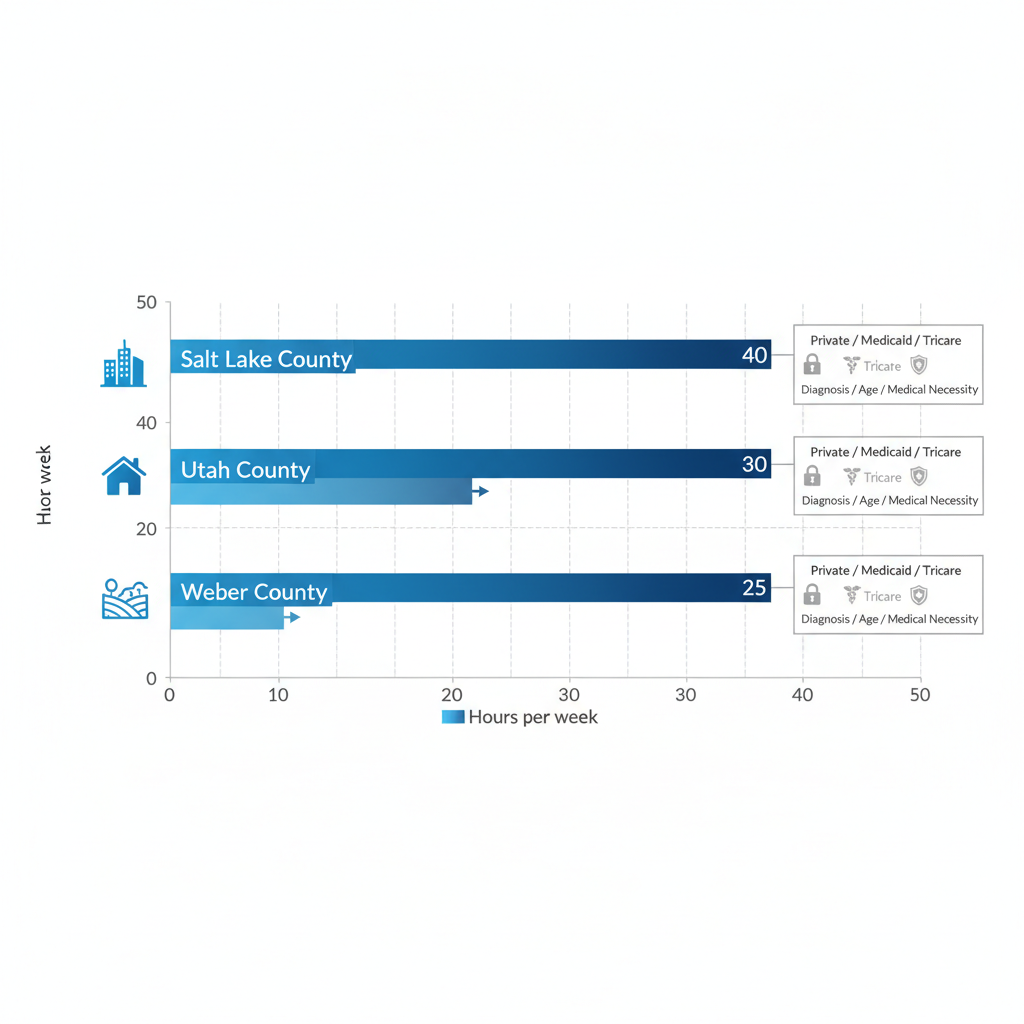
ABA Therapy Hour Limits Across Utah Counties Visualized
Insurance coverage is subject to verification and is not guaranteed–always check with your provider for the latest details.
Accessing ABA Therapy Services Across Utah Counties
Families across Utah can access ABA therapy through established provider networks that emphasize in-home delivery, ensuring comfort and consistency for children with autism. We help families navigate insurance pathways like Medicaid and Tricare, coordinating with credentialed providers who meet reimbursement requirements such as BCBA supervision and RBT implementation. This approach addresses behavioral services accessibility in Utah regions, from bustling urban areas to remote rural counties.
County-specific access varies, with robust options in Salt Lake and Weber counties where urban infrastructure supports frequent sessions. In rural areas, in-home ABA therapy remains available, though travel logistics may influence scheduling. For ‘Does insurance cover ABA therapy in Utah,’ coverage depends on plans: Utah Medicaid requires eligibility verification through income thresholds (typically up to 300% of federal poverty level) and application via the state’s portal or local offices. Under ‘Utah Medicaid ABA therapy coverage,’ families qualify for CHEC programs if children meet autism diagnosis criteria, with steps including:
- Submitting medical documentation
- Completing eligibility screening
- Awaiting approval for hours
Tricare families benefit from the Autism Care Demonstration, covering ages 0-21 with prior authorization processes outlined on official resources. ‘Tricare ABA therapy in Utah’ includes up to 25 weekly hours for active-duty dependents. Hour authorizations differ by plan:
- Private insurance: Up to 40 hours weekly
- Tricare: 25 hours maximum
- Medicaid: Variable based on need assessment
Note that insurance coverage is subject to verification and not guaranteed.
At Golden Touch ABA, we integrate seamlessly in insured ABA programs by county, offering personalized plans with family training and our interactive ABA roadmap for progress tracking. In in home aba utah county, sessions flow from assessment to goal-setting, one-on-one RBT delivery under BCBA oversight, and caregiver involvement–empowering small steps toward independence in a warm, family-centered environment.
Key Requirements and Considerations for ABA Coverage in Utah
We know how important it is for families in Utah to understand if insurance covers ABA therapy for their child with autism. To qualify for coverage, a formal autism diagnosis from a qualified professional, like a psychologist or physician, is essential. Prior authorization from the insurer is often required, involving documentation of medical necessity and treatment plans. Eligibility criteria for behavioral therapy insurance in Utah typically include age restrictions and assessments to ensure ABA is appropriate.
For ABA Therapy Utah Medicaid, the Children’s Health Evaluation and Care (CHEC) program mandates income eligibility and comprehensive evaluations. Families can apply online, by mail, or in person through the Utah Medicaid website, which offers forms in English and Spanish, plus contact details for the Department of Workforce Services. Utah Medicaid ABA therapy coverage supports evidence-based in-home interventions with BCBA oversight. For Tricare ABA therapy in Utah, coverage applies to dependents under 21 enrolled in the Autism Care Demonstration, focusing on personalized plans and progress reporting.
Key considerations include caps on therapy hours, typically 40 per week, co-pays based on plan details, and options for appeals if coverage is denied. Coverage prerequisites for autism ABA statewide emphasize ongoing monitoring to track improvements. Remember, insurance coverage is subject to verification and is not guaranteed– we’re here to help navigate these steps with family-centered care.
Steps to Verify and Secure ABA Therapy Insurance in Utah
Navigating insurance for ABA therapy can feel overwhelming, but we’re here to guide Utah families through the process. Many wonder, ‘Does insurance cover ABA therapy in Utah?’ The answer often lies in checking ABA benefits in Utah plans carefully. At Golden Touch ABA, our insurance assistance and benefits eligibility support simplifies securing autism therapy funding locally, especially for in-home ABA therapy in areas like Salt Lake County.
Follow these six practical steps to verify and secure coverage:
- Review your policy: Start by examining your health insurance documents for ABA inclusions, focusing on autism-related behavioral therapies.
- Contact your insurer: Call the customer service line or use their online portal to request a detailed benefits summary, including session limits and copays.
- Gather necessary documentation: Collect your child’s diagnosis from a licensed provider, along with any required assessments like those for Utah Medicaid ABA therapy coverage.
- Submit prior authorization: Work with a Board Certified Behavior Analyst (BCBA) to create a treatment plan and submit it for approval, noting Tricare’s typical 30-60 day timelines.
- Confirm in-network providers: Verify if your chosen ABA provider accepts your plan–options like aba therapy salt lake county often align well with local networks.
- Schedule and monitor: Once approved, book the initial session and track claims through your insurer’s system to ensure smooth reimbursement.
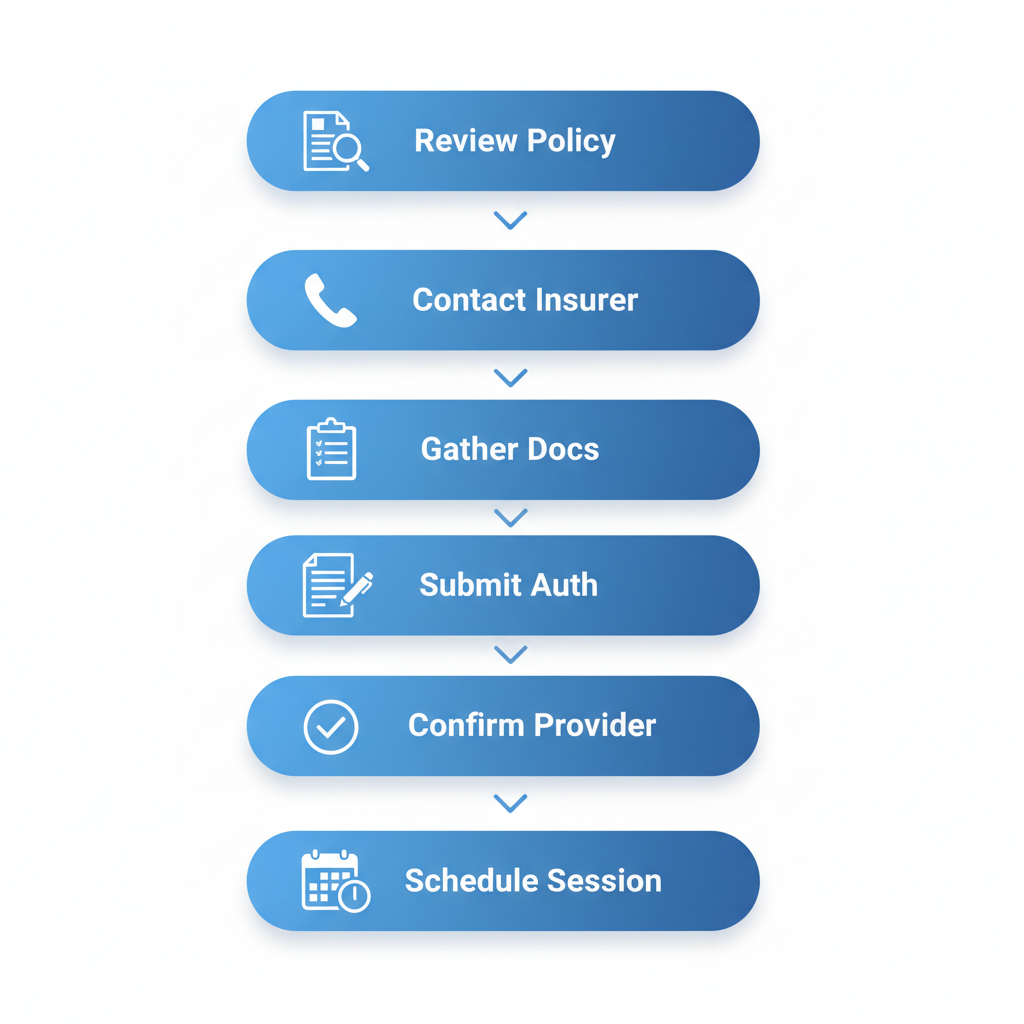
Six-step process to verify ABA therapy insurance in Utah
For specific tips, if using Utah Medicaid, leverage their Eligibility Lookup Tool with your child’s details for quick verification–Utah Medicaid ABA therapy coverage includes up to 40 hours weekly for qualifying youth, but caps apply based on age and needs. Military families should explore Tricare ABA therapy in Utah through the Comprehensive Autism Care Demonstration, requiring DD Form 2940 for authorization. We provide family-centered care to support you every step, though insurance coverage is subject to verification and is not guaranteed.
Navigating ABA Therapy Insurance: Your Next Steps in Utah
Does insurance cover ABA therapy in Utah? Yes, through state mandates, Utah Medicaid ABA therapy coverage, and Tricare ABA therapy in Utah, families can access vital early intervention for better outcomes. Promptly verify your benefits to start this supportive journey, as highlighted by Autism Speaks resources for ongoing guidance.
At Golden Touch ABA, we offer family-centered care with in-home ABA therapy, insurance assistance, and personalized assessments. Explore Utah ABA funding options and statewide behavioral therapy support–contact us today for aba therapy weber county and beyond.
